Major Policy Advances Supporting Pediatric Outpatient WGS
Today, 80% of people in the United States have access to WES, often as a second-line test, when traditional chromosomal microarray or other targeted tests have not led to a diagnosis for a patient. As payers review recent publications outlining the evidence of WGS superiority on the clinical and economic value, it becomes evident that the most efficient testing pathway to end – or better to prevent – a diagnostic odyssey for their beneficiaries is WGS access (first line in many policies). Towards this direction payers have started to offer beneficiaries access to first line WGS in patients with suspected complex genetic disease (e.g. neurodevelopmental delays) presented in the ambulatory setting, independent of age.
Outpatient coverage for WGS has greatly expanded in the last three years; approximately 70% of people in the United States who hold a commercial insurance plan will have access to WGS by June 2026. Multiple large private payers and 22 state Medicaid plans currently cover WGS. Additionally, several lab benefit managers, including eviCore, Carelon*, Avalon**, Concert and MCG cover WGS.
*Effective June 14, 2026
**Covers WGS after WES
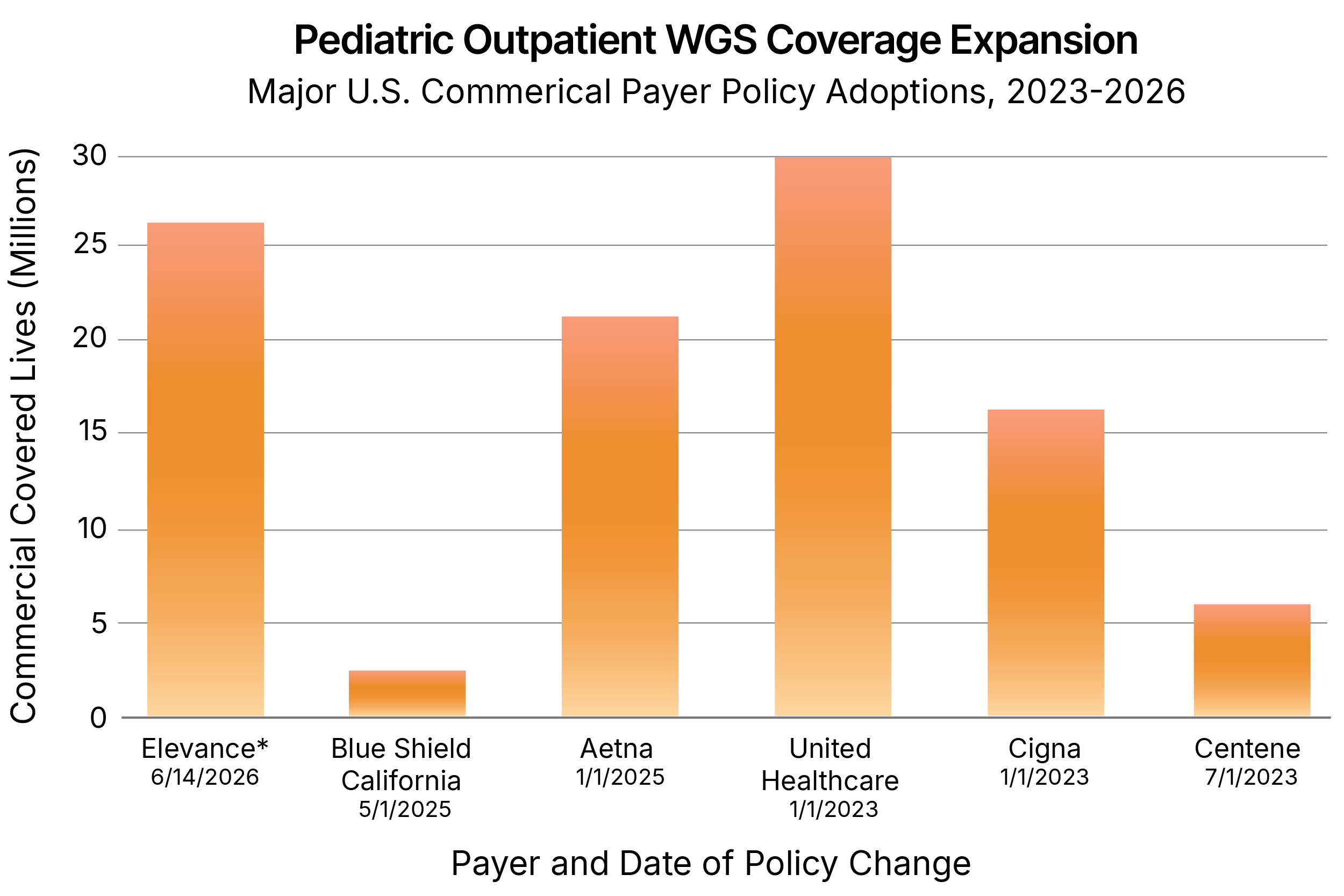
22 State Medicaid Plans Currently Cover Outpatient WGS
Approximately 44 Million Covered Lives for WGS under State Medicaid
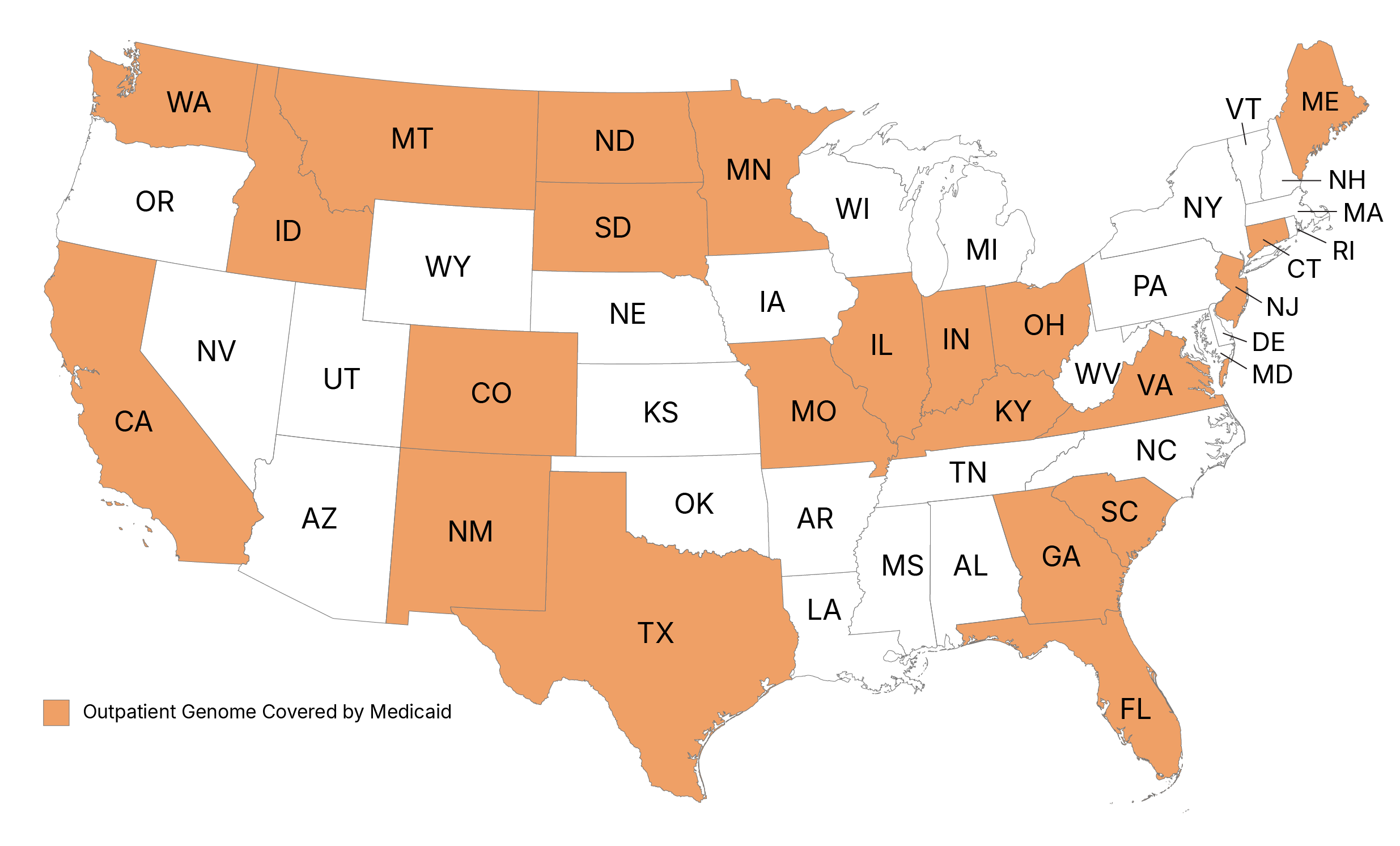
*Data on file. Data current through February 2026.
Inpatient (NICU) Coverage of rapid WGS
Coverage for rapid WGS in acute settings, such as the Neonatal Intensive Care Unit (NICU) and Pediatric ICU (PICU), is increasing as the clinical and economic value of the test build evidence across studies. Several children’s hospitals across the United States have participated in research studies to demonstrate how implementing rapid WGS in their NICU/PICUs improved outcomes including time to diagnosis, diagnostic yield, and subsequent changes to patient management.
The Rady Children’s Institute for Genomic Medicine keeps an up-to-date list of all private payers and state Medicaid plans which cover rapid WGS. A map of Medicaid coverage for rapid WGS, current through February 2026, can be found below.
Medicaid Coverage of Rapid Genome Sequencing in Acute Care Setting

*Data on file. Data current through February 2026.
To discuss additional questions regarding payer coverage with a member of the Illumina Market Access team, please send an email to: medinfo@illumina.com
The information on this website is specific to U.S. payers only. All information is based on publicly available data and is subject to individual payer policies. Contact payers directly for accurate information.


